Virtual reality is slowly making an impact in the field of medicine. From virtual surgeries to interactive 3D anatomy lessons, this technology is helping to make medicine more cost-effective and efficient, helping more individuals to become doctors and nurses. While many hospitals have already seen success using virtual reality or augmented reality, a new study from the Victor Chang Cardiac Research Institute has found that virtual reality can be used with MRI machines, creating the first-ever virtual biopsy.
Virtual Reality in Medicine
Virtual reality technology has many different applications within medicine. It can help create simulations of drug trials with patients, without needing actual live patients. Because virtual and augmented reality often use “digital twin” technology (a virtual rendering of a real-life object or location), they can also simulate the drug manufacturing process. This in turn can help pharmaceutical companies better streamline their production, helping to lower the cost of drugs as a whole. This can make these life-saving medicines more accessible for those who desperately need them.
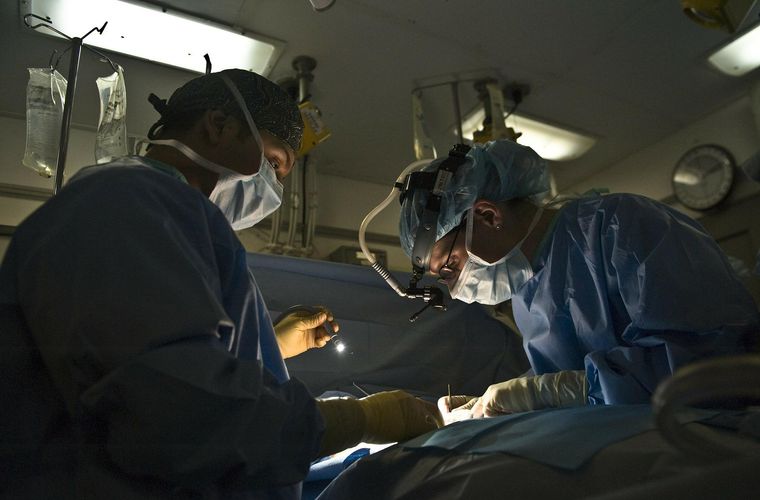
This technology is also beneficial for medical education and surgery. Using virtual or augmented reality, students can run through practice surgeries without the cost or need for cadavers. Virtual surgeries allow students to make mistakes in a safe environment, building confidence as they continue to learn. Because many practice surgeries may require a cadaver with a specific disease or problem, virtual surgeries allow for these needs to be met in an easy way. These lessons can also be better customized for a specific medical field, and help to enhance student engagement. With its many applications, doctors and hospitals are becoming more excited to test this new technology on live patients.
A Rise in Virtual Surgeries?
One place looking to use this technology is the Victor Chang Cardiac Research Institute. In a new study, published in the journal Circulation, the researchers developed a new MRI technique that has virtual aspects to it, allowing it to be less invasive on patients. The scientists tested their technique on 20 heart transplant patients, who needed these biopsies to make sure the transplant process was going smoothly. From their analysis, the researchers found their technique to be just as effective in identifying possible rejection of the new heart by the patient’s body. According to Associate Professor Andrew Jabbour of the Institute: “This new virtual biopsy takes less time, is non-invasive, more cost-effective, uses no radiation or contrast agents, and most importantly, patients prefer it.” Most normal biopsies involve an invasive process of inserting a tube into a patient’s jugular vein. From there, the doctor can use a biopsy tool to determine how the new heart is doing in the patient’s body. Because of this invasive procedure, many patients feel more uncomfortable and may even have to undergo more surgery if a complication is found, or the body is rejecting the new organ.
With around 3500 patients worldwide receiving heart transplants annually, there is a large need for this type of technology. As many of these patients also undergo about 12 biopsies in the first year after the transplant, having a much less invasive technique can not only be cost-effective for the patient but promote better recovery. The researchers are hopeful that their results will inspire others to adopt this technique. “The technique is now frequently used at St. Vincent’s hospital in Sydney,” explained researcher and cardiologist Dr. Chris Anthony. “And I anticipate that more clinics across the world will adopt this novel technology.” This technique is one of many that has illustrated the success of virtual reality within medicine and hints that this technology will continue to be applied for better success.
For more market insights, check out our latest metaverse news here.